Submitted by wcm_male_infert... on April 28, 2015 - 11:50am
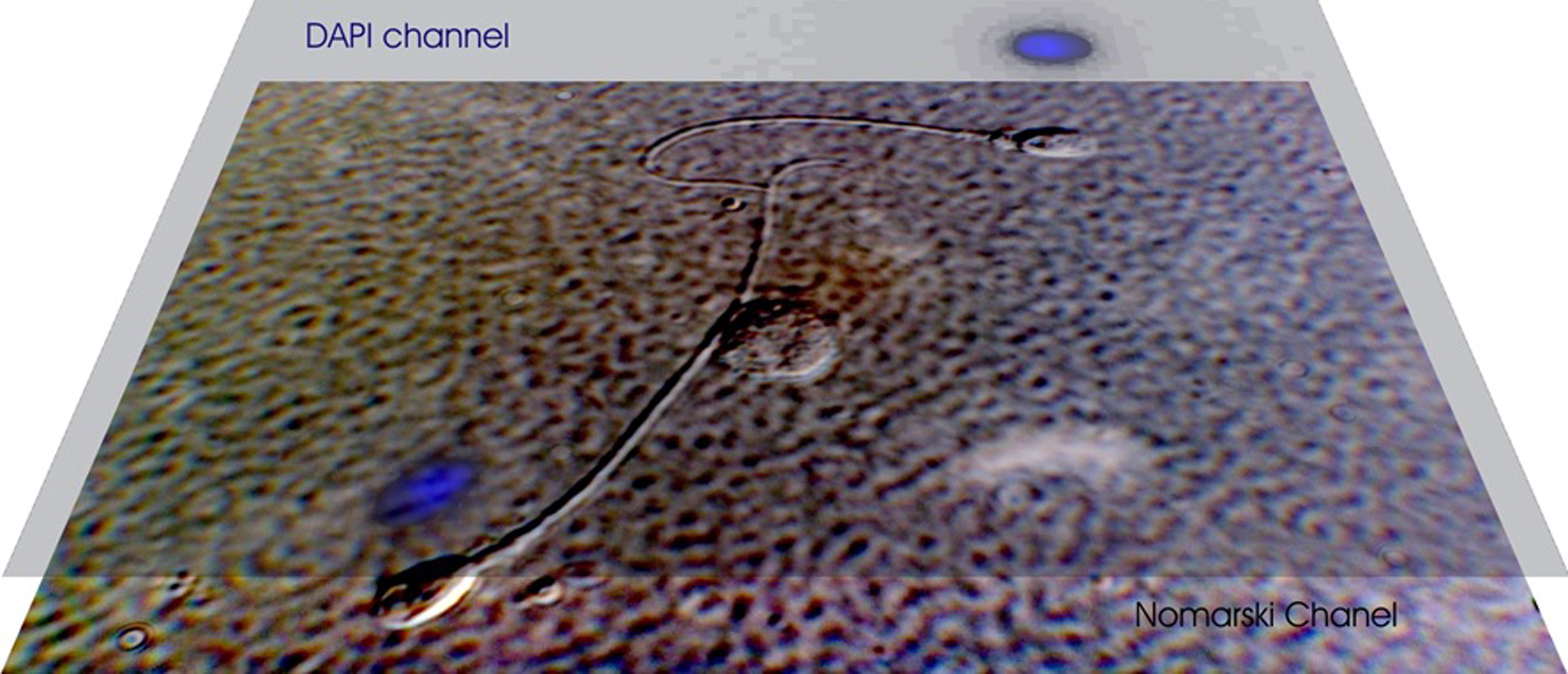
TUNEL
- The TUNEL assay is a highly sensitive and reproducible method of assessing the integrity of sperm DNA. It measures the number of breaks or nicks in the DNA of the sperm.
- It can be performed on as few as 1,000 sperm, even on sperm retrieved from a small testis biopsy.
- Other assays like the sperm chromatin structure assay (SCSA) require at least one million sperm.
- The established normal value is less than 10% of sperm with DNA damage, but in our laboratory we have shown that most men will have a TUNEL assay less than 7%. Thus our normal range is slightly lower than other laboratories.
How is it done?
- Men should have no infection in their genitourinary tract.
- Sperm from the ejaculate or testis is placed on a slide and dried out in the air.
- The sample is good for seven days if stored in darkness at room temperature.
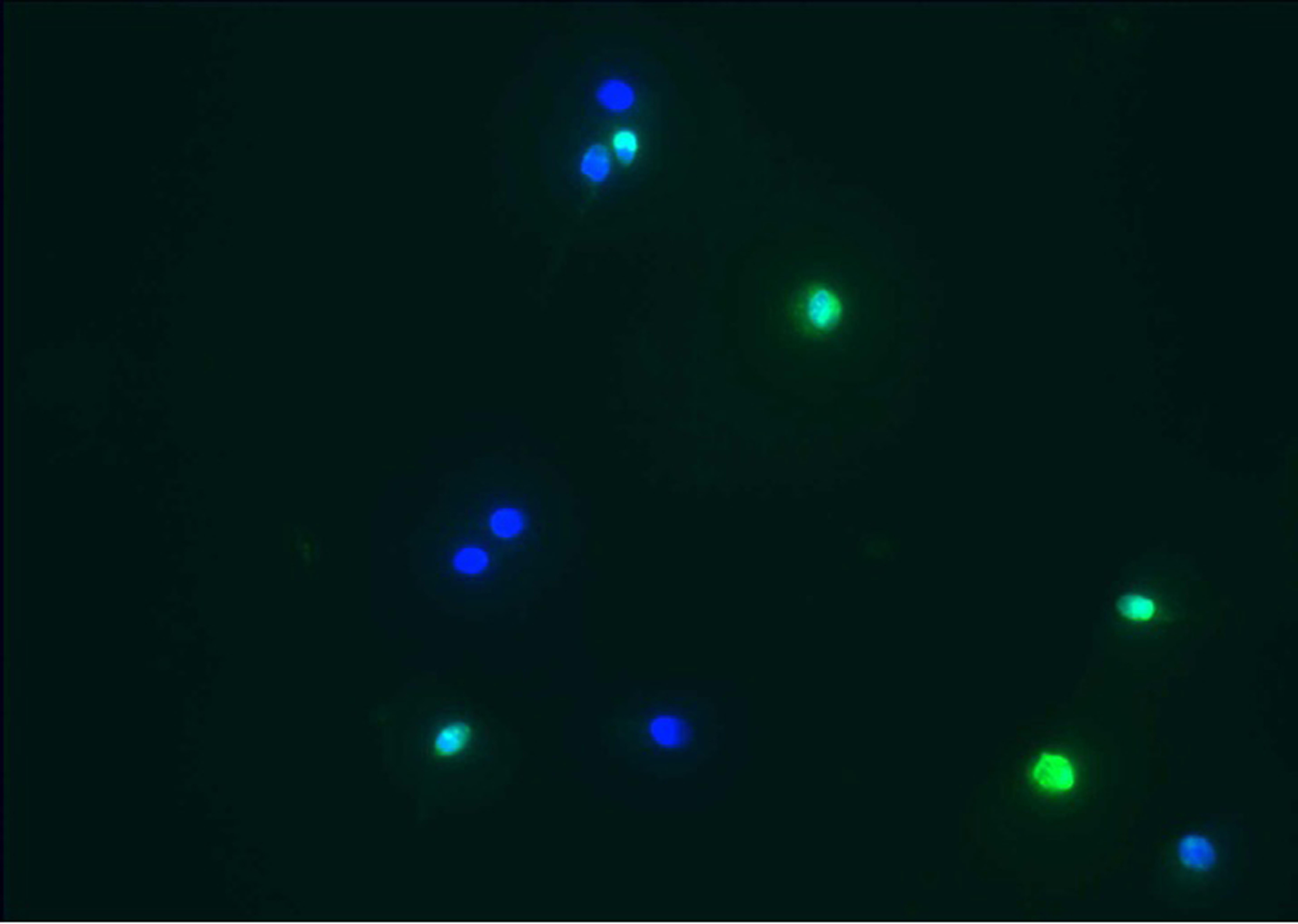
- In the laboratory, the normal sperm stain blue and the sperm with chromatin damage stain green. (TUNEL images 1 and 2)
- Results are expressed as a percentage of damaged (green) sperm to normal (blue) sperm.
- The error of measurement is below 5%.
How does the TUNEL assay help with my evaluation?
- Elevated sperm DNA damage has been associated with poorer pregnancy rates when conceiving naturally, with IUI or even with IVF with ICSI. It is also associated with increased risk of spontaneous early abortions (early loss of pregnancy). The TUNEL assay may help explain why your wife is losing her pregnancies or why IVF is failing after transfer of embryos.
- Varicocele, smoking, infections, high temperature, heavy metal exposure, chemotherapy and antidepressants have all been associated with increased sperm DNA damage. Performing a TUNEL assay can help us to determine if the medications you take or conditions you have are the likely cause of your infertility and guide our recommendations on how to best treat you.
- In our experience, men with persistent, very high (> 25%) frequency of abnormal sperm on TUNEL assay are unlikely to achieve pregnancy even with in-vitro fertilization with intracytoplasmic injection (IVF/ICSI). In such situations, you may discuss using testicular sperm for IVF/ICSI or repair of varicocele if present.
Why is my doctor recommending using testicular sperm?
- We have recently published in Fertility & Sterility (August, 2015) that sperm retrieved from the testis has much less DNA damage in men who have a very high percentage of TUNEL positive (damaged) sperm in their ejaculate.
- Using sperm from the testis in those couples who failed at least one in-vitro fertilization cycle resulted in a 50% pregnancy rate when sperm from the testis was used instead of ejaculated sperm.
- Although this study suggests that in some cases of unexplained infertility and failure of in-vitro fertilization, if semen has a very high percentage of TUNEL positive (damaged) sperm, using testicular sperm may improve the chances of pregnancy.
How many TUNEL assays have been performed in the Male Infertility Genetics Laboratory of Weill Cornell Medical College?
- The Male Infertility Genetics Laboratory is a highly specialized male reproductive laboratory with over 12 years of experience in studying and evaluating sperm DNA damage.
- Close to 1,000 assays have been performed and our laboratory serves as a reference lab for many studies, including FDA regulated studies.

